Clinical information
Coeliac disease is a systemic autoimmune disease with a pronounced genetic predisposition which may affect different organ systems. The prevalence of the disease is estimated to be approximately 1 %, but experts assume that there is a large number of additional cases that are not diagnosed due to “atypical” or mild symptoms. Coeliac disease is triggered by the consumption of gluten, which makes up around 90 % of the protein content of many cereal grains. In most cases, the disease manifests as severe inflammation and damage to the mucous membrane of the small intestine (enteropathy). In conjunction with the resulting malabsorption of nutrients, a wide range of clinical gastrointestinal and non-gastrointestinal symptoms can develop (including chronic diarrhoea, vomiting, abdominal pain, cramps, short stature, weight loss, delayed puberty, spontaneous abortions, anaemia and osteoporosis). Furthermore, dermatitis herpetiformis (Duhring’s disease), a chronic skin rash, can occur.
Both genetic and environmental factors contribute to the development of coeliac disease. Enteropathy, which is characteristic of coeliac disease, is caused by an overreaction of the immune system to gluten components, especially the so-called gliadin. Gliadin is only partially digested in the small intestine. If there are gaps in the intestinal epithelium, as is typical in patients with coeliac disease, the resulting gliadin fragments (peptides consisting of 33 amino acids, 33-mer) can pass through the intestinal barrier and reach the connective tissue underneath. There, the enzyme tissue transglutaminase (tTG) modifies (deamidates) the amino acid glutamine (Q) into the amino acid glutamate (E) at certain sites of the gliadin peptides. This modification brings on an immunological reaction in individuals with a genetic predisposition. The activation of B cells leads to the production of antibodies against the deamidated gliadin peptides and against the body’s own tissue transglutaminase. In addition, T cells secrete pro-inflammatory cytokines which cause an inflammatory reaction in the tissue. The immunological overreaction and the inflammation of the epithelium of the small intestine lead to apoptosis of the enterocytes, atrophy of the villi and widening of the intestinal crypts (hyperplasia). These damages mean that the intestinal mucosa is no longer able to absorb sufficient nutrients from the digested food and to transport them into the bloodstream.
Diagnostics
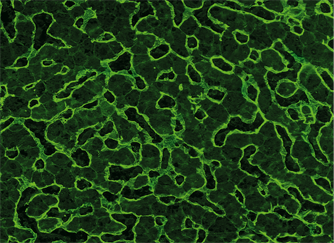 According to the guidelines of the European Society of Pediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) (Husby et al., 2020), patients with relevant symptoms should first be tested for anti-tTG antibodies (IgA) and total IgA antibodies, as these antibodies are particularly specific and sensitive. If the anti-tGG IgA is more than ten times the antibody concentration at the upper limit of normal (> 10x ULN) and a sample taken later is positive for anti-endomysium (EmA) IgA, a biopsy, which is otherwise required to confirm the diagnosis, can be omitted. The guidelines also emphasise the usefulness of coeliac-specific IgG-based tests in other cases, such as tests for the detection of antibodies against deamidated gliadin peptides (DGP). If there is a general IgA deficiency – as often observed in coeliac disease patients – anti-DGP antibodies (IgG) are considered an important alternative indicator of coeliac disease. EmA, which targets tTG as antigen, can be detected in IIFT on tissue sections of primate liver, primate oesophagus or primate intestine.
According to the guidelines of the European Society of Pediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) (Husby et al., 2020), patients with relevant symptoms should first be tested for anti-tTG antibodies (IgA) and total IgA antibodies, as these antibodies are particularly specific and sensitive. If the anti-tGG IgA is more than ten times the antibody concentration at the upper limit of normal (> 10x ULN) and a sample taken later is positive for anti-endomysium (EmA) IgA, a biopsy, which is otherwise required to confirm the diagnosis, can be omitted. The guidelines also emphasise the usefulness of coeliac-specific IgG-based tests in other cases, such as tests for the detection of antibodies against deamidated gliadin peptides (DGP). If there is a general IgA deficiency – as often observed in coeliac disease patients – anti-DGP antibodies (IgG) are considered an important alternative indicator of coeliac disease. EmA, which targets tTG as antigen, can be detected in IIFT on tissue sections of primate liver, primate oesophagus or primate intestine.
EUROIMMUN offers different ELISA, EUROLINE, ChLIA and IIFT test systems for the detection of antibodies against tissue transglutaminase, against endomysium as well as against deamidated gliadins.
Files
Test systems for coeliac disease diagostics


















 According to the guidelines of the European Society of Pediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) (Husby et al., 2020), patients with relevant symptoms should first be tested for anti-tTG antibodies (IgA) and total IgA antibodies, as these antibodies are particularly specific and sensitive. If the anti-tGG IgA is more than ten times the antibody concentration at the upper limit of normal (> 10x ULN) and a sample taken later is positive for anti-endomysium (EmA) IgA, a biopsy, which is otherwise required to confirm the diagnosis, can be omitted. The guidelines also emphasise the usefulness of coeliac-specific IgG-based tests in other cases, such as tests for the detection of antibodies against deamidated gliadin peptides (DGP). If there is a general IgA deficiency – as often observed in coeliac disease patients – anti-DGP antibodies (IgG) are considered an important alternative indicator of coeliac disease. EmA, which targets tTG as antigen, can be detected in IIFT on tissue sections of primate liver, primate oesophagus or primate intestine.
According to the guidelines of the European Society of Pediatric Gastroenterology, Hepatology and Nutrition (ESPGHAN) (Husby et al., 2020), patients with relevant symptoms should first be tested for anti-tTG antibodies (IgA) and total IgA antibodies, as these antibodies are particularly specific and sensitive. If the anti-tGG IgA is more than ten times the antibody concentration at the upper limit of normal (> 10x ULN) and a sample taken later is positive for anti-endomysium (EmA) IgA, a biopsy, which is otherwise required to confirm the diagnosis, can be omitted. The guidelines also emphasise the usefulness of coeliac-specific IgG-based tests in other cases, such as tests for the detection of antibodies against deamidated gliadin peptides (DGP). If there is a general IgA deficiency – as often observed in coeliac disease patients – anti-DGP antibodies (IgG) are considered an important alternative indicator of coeliac disease. EmA, which targets tTG as antigen, can be detected in IIFT on tissue sections of primate liver, primate oesophagus or primate intestine.